You Can Trust Your Heart in Our Hands.
Whether you’re in need of preventative care or emergency treatment, every patient that walks through our doors is treated with the highest quality of care and compassion. We provide individualized treatment plans and offer a wide range of services to help you achieve better heart health. From diagnostic testing, advanced imaging, and minimally-invasive procedures to cardiac rehabilitation, we make taking care of your heart easier than ever.
Some of the common conditions treated by our cardiologists are:
- Adult Congenital Heart Disease (ACHD)
- Blood Clot to Lung (Pulmonary Embolus)
- Coronary Artery Disease
- Heart Attacks
- Heart Valve Disease
- High Blood Pressure
- High Cholesterol
- Irregular Heartbeat (Arrhythmia)
- Peripheral Artery Disease
- Plaque Build-up in Blood Vessels (Atherosclerosis)
Cardiac and Vascular Testing
Our Heart and Vascular team offers a variety of diagnostic testing for both inpatients and outpatients. Tests ordered by your doctor must be scheduled. Tests we perform include:
EKG
An EKG is a test to determine the electric activity of your heart. Twelve leads are connected to your chest, arms, and legs via stickers (electrodes) to obtain the information needed.
Echocardiogram
An echocardiogram is a picture of the heart’s movement. During an echocardiogram, three electrodes will be placed on your chest – these are attached to an electrocardiograph (EKG) monitor that charts your heart’s electrical activity during the test. A sonographer will place a hand-held wand on your chest to get an ultrasound of your heart in order to evaluate its pumping function.
Event Recorder
An event recorder is a portable device used to record your heart’s electrical activity during symptoms as you go about your daily routine. If you have fast, slow, or irregular heartbeats (arrhythmias), your doctor may ask you to wear an event recorder.
Stress Test
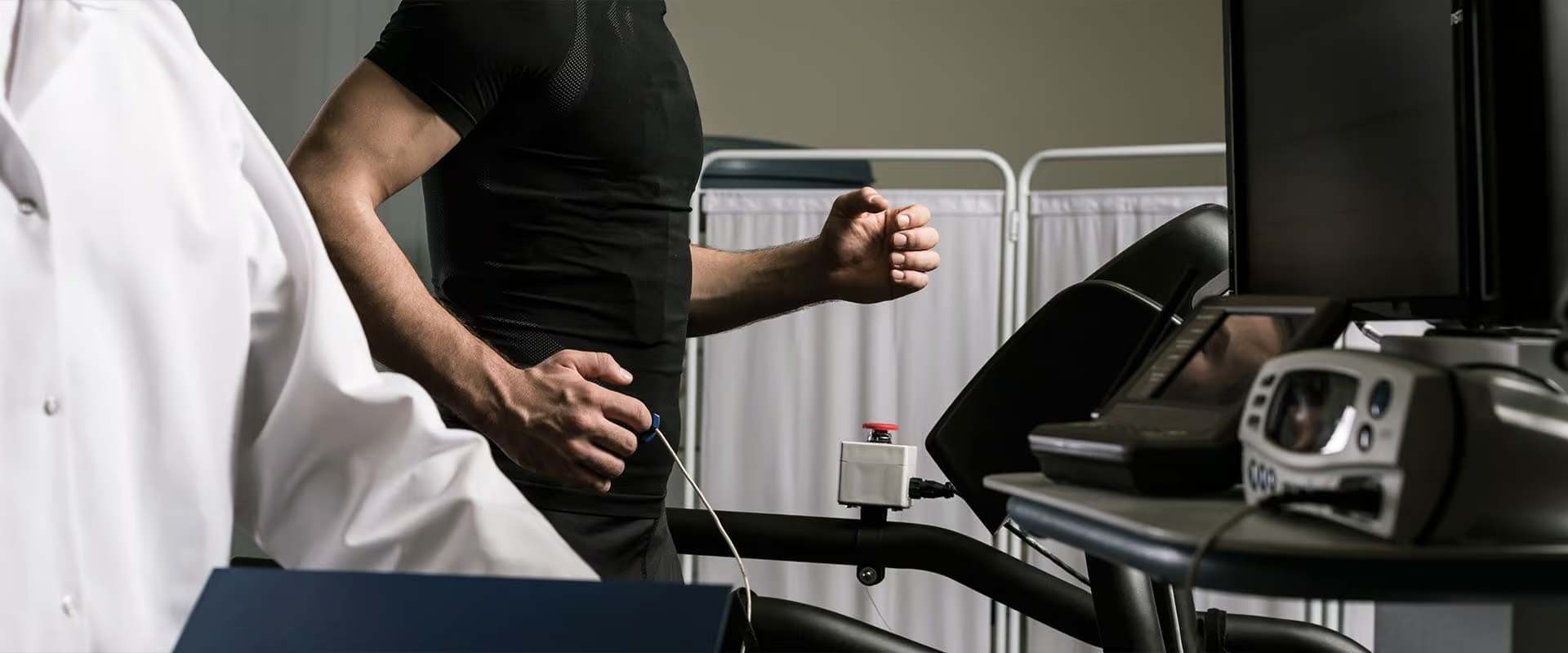
The stress test is done while you walk on a treadmill. During the test, an EKG records the electrical activity of your heart. A trained technician (or nurse) will place several electrodes on your chest and shoulders. The electrodes are connected by wires to an EKG machine with a monitor. A blood pressure cuff is applied to your arm to monitor your blood pressure. You will be shown how to step onto the treadmill and how to use support rails to maintain balance. The treadmill starts slowly and the speed and incline are gradually increased. Your blood pressure will be checked every few minutes and your EKG tracing watched for any abnormal changes. You will be asked to report any symptoms such as chest pain, shortness of breath, leg fatigue, or dizziness. The test will end when you become too tired, have significant symptoms (such as shortness of breath) or when you reach your peak heart rate.
Holter Monitor
Holter Monitoring is a continuous recording of your EKG, usually for 24 hours, while you go about your daily activities.
The holter monitor is a small portable tape recorder worn on a strap near the shoulder or around the wrist. Several electrodes are placed on your chest and connected by wires to the recorder. Your EKG is recorded and printed out. You’ll keep a diary to enter your activities and any symptoms you experience and the times they occurred. This allows doctors to detect any abnormalities and compare them to activities and symptoms.
Holter Monitoring is very safe and has no risk involved. It is only a minimal inconvenience to carry the recorder.
Vascular Tests
- Angiography
- Computerized Tomography (CT) scan
- Magnetic resonance imaging (MRI)
- Ultrasound
- X-rays
Pastor Ash
August 14th began as a normal day for Pastor Ash. He ran errands, answered emails, and completed paperwork for an upcoming conference. He was on his way to a lunch meeting when he started to feel a tightness in his chest. Having a previous encounter with open heart surgery, Pastor Ash knew the symptoms of a heart attack all too well. Being only minutes from Galion Hospital, he turned his car around and drove straight to the emergency department.

Walking into the hospital with urgency, Pastor Ash announced to the registration staff that he was having a heart attack. A nurse came quickly with a wheelchair and took him into an exam room. Within seconds, a “Cardiac Alert” was called over the intercom. Doctors, nurses, and techs filled the room. According to Ash, “one shaved my chest, one connected a portable EKG, and then a call went out to the cardiac catheterization lab, who sent a team STAT.”
Pastor Ash was wheeled from the emergency department to the cath lab and within minutes, his heart stopped once and then a second time. He was resuscitated through defibrillation. Once Ash’s heart started beating again, Dr. Joseph Mayo, Dr. Michael Davis, and Dr. Mohamad Saab were confronted with the difficult task of repairing the blocked vessel that was preventing blood from flowing to the heart. The procedure lasted several hours. While the team had collectively performed tens of thousands of heart interventions throughout their careers, this was their first case at Galion Hospital.
Galion Hospital had just opened its Level II Cath Lab at 8:00am that morning. Pastor Ash was the first patient. “If it weren’t for that moment in time, I don’t think my life would have been saved,” explained Pastor Ash. “If the heart attack had happened the day before, I probably would have died. My family and I really appreciate the care that Avita provided to save my life and bring me quickly back into functioning.”

After his procedures, Pastor Ash recovered in Galion Hospital’s intensive care unit. He was released from the hospital a few days later and is participating in Avita’s cardiac rehab program, right down the hall from the cath lab where his life was saved. Pastor Ash is back to doing the things he loves, including his pastoral duties with church and community, spending time with his wife, Peg, and their grandchildren, and riding his bike.
“God’s not done with me yet. God gets all the glory, and Dr. Mayo and his team get all the credit for doing what was humanly possible – the medical miracles!”
Procedures
We treat a wide variety of cardiac diseases using advanced techniques and procedures. Some of the procedures we perform are:
- Cardiac Catheterization – a procedure used to diagnose and treat heart and vascular conditions
- Balloon Angioplasty – using a catheter, a tiny balloon is guided through the artery and inflated to widen the opening and increase blood flow
- Stent Placement – placed using a balloon angioplasty, the stent (a metal mesh tube) expands and locks into place inside the artery
- Angiograms – a diagnostic test using x-rays to take pictures of the heart
- Aortic Aneurysm Repairs – surgery to repair a widened area in the aorta
- Plaque Removal (Atherectomy) – a minimally invasive surgery to remove plaque from the blood vessels
- Blood Clot Removal (Thrombectomy) – an interventional procedure to remove a blood clot from the blood vessel
- Inferior Vena Cava (IVC) Filter Placement & Retrieval – a small device placed in your IVC to prevent blood clots from moving into the lungs
- Implantable Cardioverter Defibrillator (ICD) Implantation – a minimally invasive procedure to place a small device under the skin of the chest to monitor heart rhythm and detect irregular heartbeats
- Pacemaker Implantation – a minimally invasive procedure to place a small device under the skin of the chest to manage heart rhythm disorders
- Heart Rhythm Monitor Implantation – a minimally invasive procedure to place a small device under the skin of the chest to monitor your heart’s rhythm for up to 36 months
Explore Our Health Library
Emergency Heart Attack Care
During a STEMI (heart attack), a short time to treatment is vital. With a 24/7 heart attack alert team and level II…
5 Numbers you need to know
Blood Pressure Blood pressure is the force of blood against the walls of the arteries. It is measured as two…
Stroke Support
Galion and Bucyrus Hospital Emergency Teams are able to work doctor-to-doctor with The Ohio State University Wexner…
Protect your kidneys, Save your heart
Chronic kidney disease (CKD) affects more than 10% of adults in the United States – more than 20 million people may…
Avita Heart Cardiac Device Clinic
Our team specializes in the implantation and long-term monitoring of your cardiac device, including pacemakers, heart rhythm monitors, and implantable cardioverter defibrillators. All of our cardiac devices are surgically implanted at Avita Ontario Hospital, keeping advanced heart care close to home.
Cardiac devices are often needed to control irregularities caused by the heart’s electrical system, such as irregular heartbeat and heart rhythm disorders. After your cardiac device is implanted, we perform regular check-ups to ensure it’s working properly. We monitor the battery status and review the stored cardiac information every one to three months after your initial appointment. In some cases, we can perform a check-up on your cardiac device from the comfort of your house using home monitoring equipment.
At the Avita Heart Cardiac Device Clinic, we utilize multiple types of cardiac devices, including pacemakers, heart rhythm monitors, and implantable cardioverter defibrillators (ICDs). We now implant Micra™ Pacemakers, too! The Micra™ Transcatheter Pacing System (TPS) is the world’s smallest pacemaker. It’s implanted directly into the heart without wire leads. To learn more about these devices, read about cardiac devices in our health library.
Contact Information
Avita Heart Cardiac Device Clinic
715 Richland Mall, Ontario, OH 44906
Phone: 419-462-4600
Fax: 419-462-4609
Hours of Operation
Closed weekends and all major holidays
Monday – Friday: 8:00am – 4:00pm